The cAnCeR jOuRnEy (so far)
Hey there, pals!
Since no one is here yet, I figured I’d sneak in and repost what I put up on CaringBridge over the last year. Deep disappointment with that platform nudged me to move into the lightweight-blog-but-mostly-a-newsletter territory, but I don’t want to send that content straight to the trash, SO – here it is, a way-too-long, was-actually-four-posts post that sort-of-covers Oct 2020 - April 2021.
Updates soon on all of this. And I’m looking forward to writing more frequently about some of the gnarlier aspects of this dumb cancer thing (among other stuff!).
About a Surgery
Originally published by Kat on Oct. 22, 2020
Hi, friends! I wanted to give a rambling update on the surgery I had two weeks ago and my recovery since. Tl;dr: it went well, and I'm doing okay!
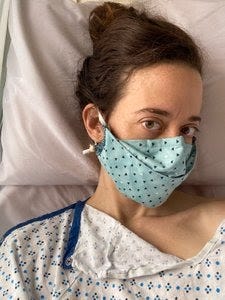
My debulking surgery (meaning: removing tumors and anything else that looks cancerous) was scheduled for Oct 8. I went in a few days prior for pre-admission testing – thanks to COVID still somehow not being under control in this country, any patient who undergoes a procedure in NY needs to have a negative a COVID test result before admission. Along with that they checked for a whole host of other things to make sure I was healthy enough for the surgery.
Well, that afternoon I got a call from my doctor. My blood count was scary low, meaning I'd need a transfusion or three before they could operate on me – I needed to get to the ER to get the ball rolling.
So, we lost two nights at home and a day we'd hoped to spend at the Brooklyn Botanic Gardens and readying the house for my recovery. Oh, well. Ask me to tell you about that night at the ER sometime. It was wild.
Thankfully, I was able to get the transfusions I needed over the course of that night and the next day, and my surgery was able to proceed as scheduled. Side note: if you have ever donated blood, THANK YOU. I realized at some point during those 36 hours that three strangers who donated theirs truly saved my life.
The day of surgery was, of course, a blur. I met the whole team, was wheeled in to the prep room, and was asleep before an anesthesiologist told me to count back from anything. I woke up hours later in the most pain I'd ever been in, but I'm gonna say it was worth it: my surgeon successfully removed my tumors, a cancerous lymph node hiding in the lining of my abdomen, along with my ovaries and uterus. I wonder: what's happening with all this extra real estate now in my abdomen?!
I stayed in the hospital three more nights, through the roughest part of my recovery. I'm forever grateful for the nurses who let Brian stay with me a liiiittle longer than visiting hours every day (and even more grateful to Brian for walking across Brooklyn every day to see me). I also now have a lot of OPINIONS about our nation's health care system and food in hospitals, but those are rants for another time.
Since getting home, I've been surrounded by softness – both physical and emotional. Brian has, of course, been an absolute dream of a partner through all of this. My folks quarantined and drove to Brooklyn to be near us, support us however we needed, and cook us lots and lots of food. I'm floored by the outpouring of support from friends and family (and some anonymous kind folks as well!).
While I still have four more weeks until I'm deemed "fully recovered," I've finally begun to come out of the post-surgery haze and feel more like myself. Next up will be sorting out what needs to happen for chemotherapy, but I'm grateful for a small window of time to hunker down in our Brooklyn nest and rest a bit before diving into the next phase of this thing.
Thanks for reading, and as always, for your love and support. This is a weird and scary time unlike any I've experienced (I've led such a fortunate life!), and it means the world to know I'm surrounded by good people who are on my team. We'll try to keep you all updated somewhat regularly going forward!
❤️K
What’s Next?
Originally published by Kat on Dec. 4, 2020
Hello again, friends and family! It’s been a while since we’ve updated you – largely because there hasn’t been that much to report as I’ve been recovering, getting a care plan (and team) in place, and trying to enjoy the eye of the hurricane that falls between surgery recovery and starting chemotherapy.
Since we last updated y’all here, I’ve continued to recover from surgery. I’ve heard a hundred times or so that recovery isn’t linear, and I’ve found that to be 100% true. Thankfully, a few weeks ago I enjoyed my first pain-free evening, and I’ve been able to start exercising again. Brian and I have been able to enjoy some long walks through Brooklyn and a random let's-dress-up-for-this-Zoom-show night. I'm so grateful for these more "normal" moments.
After some frustrating delays, we now know my official diagnosis and are finally through our second-and-third-opinion quest and have found a care team, now at Mount Sinai, that we feel great about for the next step in this cAnCEr joUrNey.
I officially have stage IIIA clear-cell carcinoma. While my cancer did leave its place of origin (my ovaries), it didn’t spread past my abdomen – which is very good news. Clear-cell carcinoma, however, tends to be platinum-resistant, meaning that chemo doesn’t always do the trick of hunting down and killing those cancerous cells. Recurrence tends to be higher for this type of ovarian cancer, too. But I’ve learned to keep my calm around scary statistics: all the numbers you’ll find when late-night Googling are averages. My age and general health have my doctors, and me, a little more hopeful.
While my surgeon removed all of my visible cancer, I still need to go through chemotherapy. My new oncologist described it this way: “while they got all of the cancer out of your body, there are likely still cancerous cells floating around trying to find a place to call home. We want to catch those before that has a chance to happen.”
So – while we’re here, let’s talk chemo!
I’m on a regimen commonly referred to as carbo/taxol comprised of two chemo drugs: carboplatin and paclitaxel. I’ll get infusions of these drugs once every 21 days for six cycles. Since I just started yesterday, I expect to be done on March 18.
I had my first infusion yesterday at Mount Sinai’s Chelsea center. The space itself is light and airy - it was the first visit I’ve had where my blood pressure and heart rate didn’t spike with anxiety, which says a lot about the quality of both the center's design and the people there. Turns out: these things matter!
I got my own little private room for the day, which was really nice. The staff at the infusion center were nothing short of wonderful, and other than deep exhaustion, I didn’t have any wild reactions to the chemo. Other symptoms will pop up in the next week or two as the chemo works its way through my system (including hair loss), but I’m grateful that my first day on the drip was a good one.
But, my dear friends and family, having cancer in the middle of a raging pandemic is tough. The already-difficult things are so much harder for so many of us.
I can’t have any visitors while I’m being pumped with these toxins for 6 hours. Volunteers can’t spend time with patients in the infusion center. It seems impossible to get acupuncture or massage because with a compromised immune system I can’t risk being in a room with a stranger for more than 10 minutes, even if we’re masked. I don’t know what my doctors’ and nurses’ faces look like below the eyes - and they don’t know mine.
And now, for a moment on my soapbox
While I’m glad my center is taking Covid seriously, it’s infuriating that this administration made this a political war rather than, you know, a public health crisis, and convinced so many people that this isn’t real. I’m so mad that at this point Americans have been given a few dollars a day to get through this, and people have to work in unhealthy situations.
But that’s where we are. So please, I know it sucks, but wear a mask. Consider avoiding travel, yes, even at Christmas. Find creative ways to connect virtually. Because so many people are going through hard isolating stuff anyway, and this makes it so much heavier. We’re close to a vaccine. Staying home for a few more months and having kinda-sad, distanced holidays means we can all be together next December. Isn’t that worth it?
And yet with all of the challenging parts of this, I’m grateful for the good folks in my life who are on my team and getting me through this... even if we can’t hug til after it’s over. That’s gonna be a great day.
Lots of love to all of you. Thanks for being on my team!
💗
P.S. If you use Instagram, feel free to follow me there at @katkingmusic. I occasionally post pictures and/or small videos there about normal life, music, and now: cancer!
Let’s Talk About Chemo
Originally published by Kat on Feb. 19, 2021
Howdy pals, and a very belated Happy New Year.
I wanted to pop in for another update as I am officially more than halfway done with my chemotherapy treatment!
Too long, won’t read?
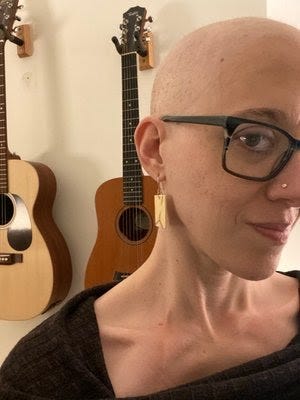
I’m doing well, all things considered! I've lost almost every hair on my head and a lot of my eyebrows/lashes. I’ve been able to handle the other side effects of my treatment pretty well and, because my infusions are spaced three weeks apart, I’ve been lucky enough to have at least a week (often two) of feeling relatively good between them! I’ll have two more infusions before we close the book on this chapter of my treatment.
Going into this thing I thought that the days I get my infusions would be ones I dread, but I’ve actually found that I don’t mind the day of my chemo treatment at all. There’s predictability! I’m surrounded by medical professionals! And they give me enough drugs that I don’t feel sick the day of treatment!
A standard treatment day
I pretty much live without an alarm clock these days, but I want to make sure I’m up with plenty of time to have a morning for myself before heading in for treatment, so my alarm wakes me up by 5:15am. I roll out of bed and shuffle into the living room where I drink water and then do 20-30 minutes of yoga followed by a guided meditation. Making both of these a priority help prepare my body and mind for the day (and week) ahead. Then I’ll shower, get dressed, and make sure Brian is awake. We’ll have coffee or tea together and I’ll down a smoothie and protein shake (I’ve found that I have no stomach issues during treatment if I start the day with a liquid diet).
We call a Lyft by 7:45am to take us into Manhattan (sidebar: I cannot wait to take the MTA again post-vaccine). We arrive at the infusion center around 8:30am and I kiss Brian goodbye since companions still aren’t allowed in the facility due to COVID. He’ll spend the day walking and taking care of errands. Yes, you’re right, he is the absolute best. ❤️
I head into the building, check in, then head to the lab where they take my blood to see how my body is handling the treatment. My oncologist watches these numbers (especially platelet, white and red blood cell, and neutrophil counts) every three weeks to make sure that the chemo isn’t poisoning me too much! I’ll be called in to the infusion center and shown to my recliner while they wait for the results of the labwork. Someone comes by to check my weight, blood pressure, temperature, and pulse.
If the lab work comes back healthy “enough,” a nurse hooks an IV up to my port and starts me on my pre-meds: a handful of drugs that will help manage the most common and disruptive chemo side effects (nausea and allergic reaction being the two big ones). After that, we run my Paclitaxel (commonly called “Taxol”) drip for 3 hours, followed by Carboplatin for 1 hour. My nurse places a Neulasta injector (more on this later) on my belly before they unhook me from the drip and send me home.
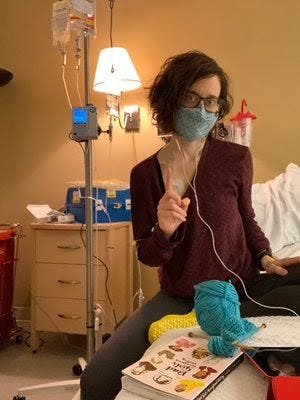
Ultimately, these days have been largely long and a little boring – I spend my time knitting, listening to podcasts, and loopily texting friends once the IV Benadryl hits.
Once I'm all done with my infusions, my friend Kelley picks me up from the infusion center and drives me home because she is the salt of the earth. It’s so great to not have to worry about being loopy or potentially sick in a Lyft, and it always lifts my spirits to see her and Brian right after leaving the building.
We’re usually home by 4pm, and I’m still buzzing from the steroids they give me as part of my pre-meds! That buzz typically lasts at least 24 hours before The Big Crash.
While my physical side effects vary session to session, it usually looks like: a few days of nausea and extreme fatigue. Maybe a week or so of bone pain (yes, bone pain) which is a side effect of Neulasta, a drug I’m given that helps my body rebuild white blood cells typically ravaged by chemotherapy.
Where we are now
Having completed 4 rounds of chemo, I finally feel like I am halfway through this part of my treatment. You might be thinking, “Uhhhh Kat half of six is three weren’t you halfway like a whole month ago? Did you fail math a lot as a youth?” to which I say I understand your confusion but no, I actually did pretty well at math. But this is a coping mechanism, not math.
Up until my third round of treatment, I had that same mindset: once I get pumped full of medical-grade poison three times, I will be halfway “done.” But then I got home and realized that, even after my final treatment, there’s at least a week of side effects to get through.
And then my fourth infusion had to be delayed a week. I went in for treatment and everything was the same as it ever was, up through the “get settled in my recliner and wait for the nurse to start my pre-meds.” Long-ish story short, my platelet count had fallen too low for me to safely get chemo. I was sent home to rest for another week before trying again.
I was, truthfully, pretty devastated. I knew this was a possibility (and have since learned that it is incredibly common on my cocktail of drugs), but it still pulls the rug out from under you. I realized that I kind of like my chemo days because it’s the one day I feel like I am actively doing something to counteract this cancer. Being sent home reminded me that I’m not even in control of that. Letting go of the need to control everything is definitely a lesson I am learning on a much deeper level this year. I went home for a week, went back the next week, and my numbers were back up to where they needed to be.
How "am" I???
This is a strange and complex question to answer these days! I completed my fourth round of chemo one week ago. For the most part each cycle has gone relatively smoothly – the five days after an infusion are usually pretty rough with fatigue, nausea, and pain, but it varies with each treatment. Drinking a lot of water – I’m talking 4 liters minimum – and exercising regularly are the two things I can do that make a notable difference in how hard those side effects hit me. There’s a cumulative effect to the drugs, so while I feel better over time they still wreak havoc on the cellular level – which is good, but it means there’s still a lot of unpredictability. I'm learning to hold hope and uncertainty hand-in-hand.
That said, I’m so glad to have a few weeks of feeling good between my infusions! I’m able to visit the botanic gardens, go for long walks, dress up for Zoom comedy shows, and work on music*, which all do a lot to help me feel fully human.
It's a little tough to not know if or how well the chemo drugs are attacking any cancerous cells that linger. For now, I just have to stay the course and trust that we'll have good news on the other side of this.
What’s next?
I have two more scheduled chemo infusions before I complete this part of my treatment. If they’re able to go as scheduled, that means March 25 will be my last infusion. As far as what happens after that… we’ll have to wait and see! I’ll focus on healing for the months that follow, as the chemo will have decimated a lot of my good cells along with the bad. My oncologist will order some tests and we’ll see if any cancerous cells remain. I’ll keep y’all posted!
💜, K
*I had a lot of fun last week collaborating long-distance with a pal of mine who lives in New Orleans! You can check out the video here.
NoMoChemo - for now (and the great unknown)
Originally published by Kat on April 2, 2021
Yesterday, April 1, I finished my chemo treatment with my 6th of 6 infusions. 🎉
I’m so relieved (and tired). I made it through this really difficult part of my cancer treatment. With treatments delayed multiple times, I'm extra glad that we were able to do my final infusion this week – while waiting another week would have been fine, I'm so glad I don't have to. But my platelet and white blood cell counts were in a healthy-enough range, and we did it! I got home, tired and relieved, to find a delightful celebratory treat (peanut butter m&ms, the very best) waiting for me (thanks, Brian 😍). We celebrate all the things whenever we can now – I highly recommend it.
I’m feeling hopeful about a brighter, not-too-distant future.
A lot of people have asked how I feel about finishing chemo. In the last week I've felt a multitude of emotions, from excitement to disbelief to fear, peace, anxiety, and more. Not exactly what I expected I'd feel like on the other side when I started treatment back in December.
But a big thing I didn't realize back then was that this is not the END. I'll be dealing with side effects of treatment for the next week or more before I can really think about celebrating. Then, we'll do a scan and follow-up with my oncologists to see if there’s any trace of cancer left in my body.
If we get a good outcome on that scan, I'll be declared "NED," or No Evidence of Disease. If I'm not... well, we'll deal with that dragon when we get to it. But ovarian cancer also has a high rate of recurrence - that mountain lion* might show up again any time. So my care team and I will need to watch things closely for the next months/year/years.
I’ve been working on holding multiple conflicting emotions at once this year. I’m learning to love these little emotion-skirmishes:
I’m so glad this chemotherapy treatment is done. I’m still pretty heckin’ bummed that I got cancer this year, to be HONEST. I’m so grateful for the health I DO have that helped me get through the doses of helpful poison the last 4 months. I’m dreading how tired/sick I may feel for the next few weeks. I’m wildly thankful for everyone who’s supported me, helped me emotionally and tactically, cooked for me, sent a card or treat, cheered me on. I don’t love not knowing exactly what comes next. I’m overflowing with love and gratitude and anxiety and calm and more emotions than my chemo brain can name.
But mostly? I’m wild with gratitude that I've found a team of good doctors, family, and friends who support me in a dozen different ways. You help balance the hard parts of this 💜
I’m glad to be on the other side of this piece of my ~cAnCeR JoUrNeY~, even if it is still scary.
Qué será, será.
What’s next?
Now we wait a little bit longer. So much of having cancer is waiting. Heal up, start getting stronger again, and have that scan and some follow-up appointments. Hopefully, we get good news and I’ll be able to live a little bit more new-normal life by the summer – made even more exciting now that I'm vaccinated against Covid!
I should know more within the month, and I'll update y'all when we know more. Hope and fear will bounce around my brain for the rest of my life, but realizing that change is the only constant in life has begun to ground me.
Heaps and heaps of love, pals. Thank you from the bottom of my heart for your love and support.
*This is one of my favorite analogies I've found around receiving a cancer diagnosis and what follows.